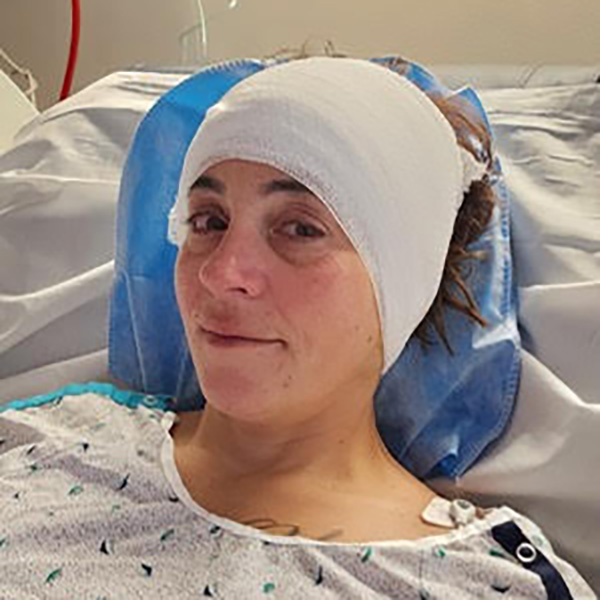
Less than a year after being diagnosed with meningioma, Amanda D. found herself walking along the Asbury Park Boardwalk with her husband, three daughters, and a close friend. As they took part in the National Brain Tumor Society’s New Jersey Brain Tumor Walk, they paused to watch dolphins playing in the ocean.
This unexpected moment brought tears of happiness, as it was a reminder of how far she had come after years of unexplained symptoms.
“My daughters and I saw all the people and ages who are affected by brain tumors at the event,” Amanda said. “And it emphasized how lucky we are that I’m still here.”
That day on the boardwalk also reinforced Amanda’s desire, since her diagnosis, to help others better understand brain tumors and the tools that can help guide informed decisions about care.
“We need more awareness of biomarker testing,” Amanda said. “It’s one of the reasons why I’m advocating for the National Brain Tumor Society, so we can increase education about brain tumors.”
Her Meningioma Diagnosis
Amanda’s passion is rooted in years of uncertainty due to unexplained symptoms. Since 2018, Amanda experienced headaches and dizziness, yet repeated brain scan results had not yielded any answers. Five years after her symptoms began, Amanda suffered her first-ever seizure, but the hospital admission and neurological workup, including a brain scan, did not reveal any abnormalities.
In August 2024, Amanda had another seizure while feeding her chickens in the backyard. Her security camera caught the seizure, so she saved the recording and took it with her to the hospital. It was after this scan that Amanda was finally diagnosed with a brain tumor.
“All these years, I just kept getting pushed off or considered like a hypochondriac,” Amanda said. “And it was a brain tumor this whole time.”
Given the challenges she faced in finding the tumor, Amanda took the discs from all of her scans since 2018 to get a second opinion about what she should do next.
“The doctor was able to pull up a picture from every disc, and the brain tumor had been there since the first scan,” Amanda said. “It was smaller and had since grown, but it was there.”
Biomarker Testing
Amanda considered her treatment options and elected to undergo brain surgery to resect the tumor. After the decision was made to operate, Amanda took steps to sign an advance directive, provided by her hospital, and verbally communicated her desires in lieu of a drafted will.
Her neurosurgeon successfully removed the 0.8-mm tumor, which is about the size of a green pea, and determined it to be grade 1 meningioma.
As part of her operation, the neurosurgeon used a dural graft to close the opening in her dura mater — the “tough outer layer of tissue that covers and protects the brain,” according to the National Cancer Institute — to prevent cerebrospinal fluid (CSF) leaks.
The neurosurgeon sent her tumor tissue out for biomarker testing, which included a gene sequencing panel that looked at the 30 genes most commonly associated with brain tumors. About two weeks later, she received the biomarker testing results at the same appointment where they removed her staples.
Her meningioma tumor had an NF2 mutation, which they explained meant she had a slightly higher risk of the tumor returning. At the time of her biomarker testing, her doctors were unsure whether it was specific to just her tumor or if it was due to a broader genetic condition called neurofibromatosis type 2 (NF2). Amanda later met with a geneticist who informed her that it was an NF2 gene mutation specific to her tumor’s makeup and not the genetic condition.
“Biomarker testing gave me a big sense of relief that I don’t have to worry about my daughters having this genetic condition,” Amanda said. “It was also reassuring to know that I’ll be getting yearly MRIs since tumors with the NF2 mutation can come back.”
To understand why these results mattered so much, it helps to know more about the NF2 gene.
NF2 Gene Mutation
NF2 gene alterations are the most common genetic abnormality in meningiomas. Research published in the International Journal of Molecular Sciences found that 50-60% of meningiomas involve either an inactivating NF2 mutation or loss of chromosome 22, where the gene is located.
Knowing whether a tumor has an NF2 gene mutation can help patients and their providers make informed decisions about their care. That’s why understanding the tumor’s biomarkers is so important and why NBTS launched MyTumorID to help raise awareness about the importance of biomarker testing for people with brain tumors.
NF2 Genetic Condition
Some meningiomas are associated with a genetic condition called neurofibromatosis type 2 (NF2). People with NF2 are more likely to develop multiple brain tumors, including meningiomas and vestibular schwannomas, due to mutations of the NF2 gene, which normally helps control cell growth. When this tumor suppressor gene isn’t working properly, it can lead to tumor development.
In patients with NF2, meningiomas are often more aggressive. Another International Journal of Molecular Sciences article notes that 50-75% of people with NF2 develop meningiomas, which are more likely to be grade 2 or 3. These meningiomas have a worse prognosis and higher recurrence rate than sporadic meningiomas.
Ki-67 Proliferation Index
Amanda’s biomarker testing also included her tumor’s Ki-67 proliferation index. Her meningioma tumor had results of less than 1%, indicating slow cell division.
The National Cancer Institute describes the Ki-67 proliferation index as a “way to measure how fast cancer cells in a tumor are dividing” since Ki-67 is a protein that is only found in dividing cells. A high score indicates that the cells are dividing quickly, which can make it more likely for the tumor to grow and spread.
In meningiomas, the Ki-67 index results have widely been used as a predictive marker for the chance of meningioma recurrence. A 2025 Journal of Neurosurgery article revealed more complexity with how Ki-67 is expressed in meningiomas; however, it stated that “the Ki-67 index remains a reliable parameter for assessing the clinical, molecular, and prognostic characteristics of meningiomas on careful evaluation and consideration of potential confounding factors.”
Looking Ahead
Today, Amanda deals with speech challenges and migraines. She remains committed to fundraising for the National Brain Tumor Society and advocating for greater awareness and education, especially around biomarker testing.
“Biomarker testing helped me understand my tumor, eased fears for my daughters, and gave me confidence in decisions about my care,” Amanda said.
Through programs like MyTumorID, NBTS is working to ensure more patients can receive the clarity Amanda did — because understanding a tumor’s biomarkers can change everything.