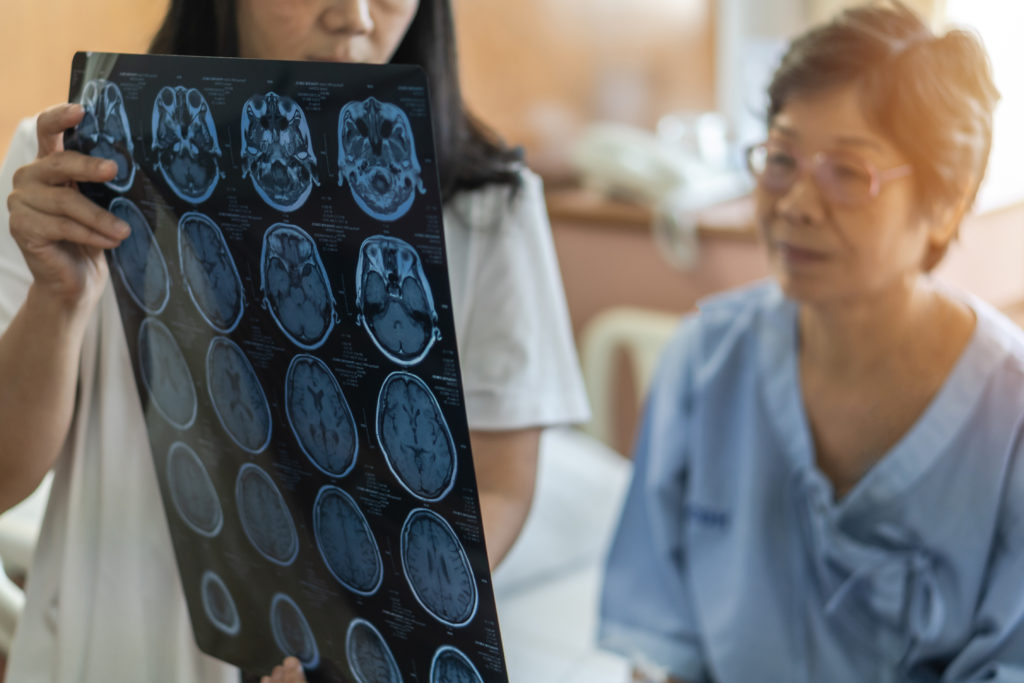
For a patient with a brain tumor, undergoing surgery is often a significant step in the treatment process. The specific experience can vary depending on the type, size, and location of the tumor as well as the overall health of the patient.
Questions to Ask Before Surgery
National Brain Tumor Society created a list of key questions to ask before having surgery, including questions to specifically ask one’s health care team and neurosurgeon. NBTS recommends patients and care partners bring these questions to their appointment either on the phone or as a printout.
Once diagnosed with a brain tumor, a health care team may recommend surgery as soon as possible if the patient is deemed a candidate for an operation. There are benefits of expedient surgery, negatives to delaying surgery, and benefits to delaying surgery to explore additional options.
If a patient’s situation allows for it, securing a second opinion can help make a more informed decision before undergoing surgery. Unsure where to look for a second opinion? Contact NBTS’s Personalized Support and Navigation team to request quality, unbiased information and resources.
Biomarker Testing
As part of surgery, biopsied samples or surgically resected portions of a tumor may undergo a process called biomarker testing. A neurosurgeon may know whether the tumor is benign or malignant — possibly even the tumor type itself — but pathology done after surgery will ultimately provide an accurate diagnosis, prognosis, and treatment options.
“They also told us that surgery is when they would let us know what type it was,” said LaTresa D., whose husband was diagnosed with glioblastoma. “It could be benign. It could be malignant, and we wouldn’t know until after the operation. They were very kind and explained things, but it was still confusing because we had never gone through it.”
More so than ever before, patients need to understand the molecular makeup of their tumor through biomarker testing to make informed decisions moving forward. Patients are encouraged to reference NBTS’s list of key questions about biomarker testing and ask these questions to their health care team before surgery.
Pre-Op at the Hospital
Once surgery has been scheduled, carefully follow the hospital’s pre-op instructions, including what to do or not to do in the 24-48 hours prior to surgery. These instructions can vary by health system, so it’s vital to refer to the patient’s specific pre-op instructions. Patients will also likely have to undergo a preoperative MRI prior to surgery.
If possible, bring your advance directive(s), which can include one’s living will and health care proxy form. These documents help patients articulate their preferences and values for future medical care when the patient is unable to make decisions for themselves, such as under anesthesia for brain surgery.
Once the patient arrives at the hospital for brain tumor surgery, they can expect the following activities and procedures at the hospital to ensure their safety and readiness for the upcoming procedure:
- Changing into a hospital gown and removing jewelry, contact lenses, and other items that could interfere with the operation
- Having an IV line placed to administer fluids and necessary medications before, during, and after surgery
- Undergoing pre-operative testing or lab work, if needed, to assess the patient’s current health status
- Meeting with the anesthesiologist to address any patient concerns and review any allergies or sensitivities to anesthesia medications
- Meeting with the neurosurgeon to discuss the surgical plan, potential risks and complications, and answer any last-minute questions
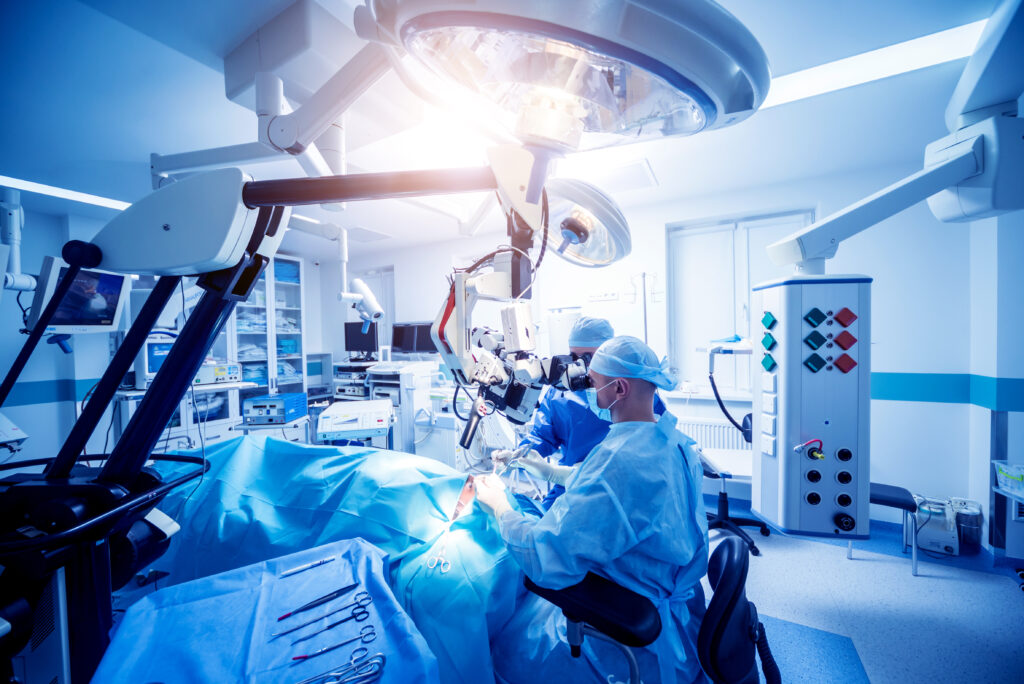
During Brain Surgery
The neurosurgeon will perform the surgery to remove as much of the tumor as possible or take a biopsy for further examination. The extent of tumor removal depends on various factors, including the tumor type, its location, and the risks associated with its removal.
Awake vs. Sedated Craniotomy
A craniotomy is a surgical procedure in which a bone flap is removed from the skull to access the brain. It is a common neurosurgical technique for various brain-related conditions, including brain tumor removal. A patient’s experience and the length of their surgery will vary depending on tumor location, type, and complications heading into surgery.
Depending on the tumor’s location, a neurosurgeon may determine that an awake craniotomy is needed rather than the traditional sedated craniotomy, where the patient is fully unconscious under general anesthesia.
In an awake craniotomy, the patient is awake and aware during parts of the surgery. This technique is often used when the brain tumor is located in an area that controls essential functions, such as speech, vision, or movement. By keeping the patient awake, the surgical team can monitor their neurological responses and ensure that critical brain functions are not compromised during tumor removal.
“An awake craniotomy gives the surgeon really good feedback in the moment instead of just a before and after picture,” said Nate Somes, MS, CCC-SLP, of the Massachusetts General Hospital (MGH) SLP Brain Tumor Team.
Craniotomy vs. Transsphenoidal Surgery
The main difference between a craniotomy and a transsphenoidal surgery lies in the approach and the areas of the brain they target. A craniotomy involves creating an opening in the skull to access various regions of the brain. Transsphenoidal surgery is a specialized approach to access the pituitary gland and nearby structures through the nasal cavity and sphenoid sinus. This type of surgery is commonly used to remove pituitary tumors. The choice between these procedures depends on the tumor’s location within the brain.
“We had planned on doing a transsphenoidal surgery until the day before my surgery,” said Gabe R., who was diagnosed with craniopharyngioma and has undergone two surgeries. “I was devastated because, to me, a craniotomy just seemed way more invasive, but my surgeon told me my downtime would be less. He was right. My recovery from the craniotomy was half of what I experienced in the transsphenoidal surgery.”
Post-Op Recovery
The patient will be taken to the recovery room for monitoring immediately after surgery. Once they are awake and their vital signs are stable, they will be transferred to a hospital room for further recovery.
It’s important to note that every patient’s experience and recovery are unique. The medical team will work closely with the patient to provide personalized care and support throughout their recovery. Additionally, recovery and rehabilitation may vary depending on the extent of surgery and the overall impact on brain function. The health care team may recommend physical, occupational, or speech therapy to aid recovery and improve quality of life.
Waking Up From Brain Surgery
Waking up from brain surgery can be a disorienting experience, and the specific sensations and feelings can vary. Some patients may feel confused or have trouble recalling recent events immediately after waking up. This confusion is often temporary and improves as the effects of anesthesia wear off.
“It’s a very surreal experience waking up from brain surgery,” shared Dace H., who has a grade 3 anaplastic astrocytoma. “Now, having done it twice, there’s like a dissociation from your own body. It feels like you’re just kind of like this floating consciousness. It’s very strange and hard to explain.”
In addition to experiencing disorientation, facial paralysis or motor changes can have a significant emotional impact on the patient upon waking up. They may feel anxious, scared, or overwhelmed by the sudden physical limitations and the uncertainty about their future abilities.
“They tell you about all the risks, including facial paralysis, before surgery, and you have to sign the consent,” said Kayla S., an acoustic neuroma survivor and now a neuro ICU nurse. “I woke up, and I could feel that my face was messed up. I immediately started crying because reality hit.”
As a neuro ICU nurse and a former patient who had a craniotomy in 2021, patients frequently ask Stacy Pietrafitta how much pain to expect after surgery.
“The day of surgery, you’ll come out a bit disoriented and drowsy secondary to your anesthesia,” Stacy shared. “You should be pretty sedated, and they’ll wake you up, but you shouldn’t be in too much pain because of your anesthetic.”
Some hospitals will offer standing pain management, providing pain medication at a designated time interval instead of as needed. If a patient’s hospital does not offer it as needed, Stacy encourages patients to ask if standing pain management is an option for them.
“You should consider asking for pain medication every four hours because your pain might be creeping up, but you don’t realize it,” Stacy explained. “If you had surgery in the morning, you can expect incisional pain by that night.”
Nausea is a common side effect that some patients may experience after brain tumor surgery. The surgical procedure, the anesthesia used during surgery, and other factors can contribute to postoperative nausea. However, not all patients will necessarily experience nausea, and the severity and duration of nausea can differ from person to person.
“I was very nauseous throughout my stay,” Stacy shared. “It was one of my complications, and I just couldn’t keep anything down.”
Patients should voice their concerns about nausea to their health care team to see if they can adjust their care plan as needed to improve comfort and provide support.
Post-Op Day One
If a patient doesn’t experience any complications during their surgery and their blood pressure and heart rate are stable, Stacy shares that her patients are typically encouraged to get up and move the next day to prevent complications and to see how their body responds to movement.
While the timing of when patients can leave the hospital for either home or a rehab center is based on the individual circumstance, tumor location can help predict potential therapy needs after surgery, including inpatient therapy.
“If the tumor is in the cerebellum, your balance is going to be affected, and you may need physical or occupational therapy in that area,” Stacy said. “If your tumor is in one of the temporal or parietal areas that affect speech, you might be able to walk but struggle to get your words out and need speech therapy.”
Hospital Stay
The length of hospital stay will depend on the surgery’s complexity, the tumor’s size and location, and the patient’s overall health. Some patients may need to stay in the hospital for a few days or longer.
After being discharged from the hospital, the patient will need to attend follow-up appointments with their neurosurgeon and neuro-oncologist for wound care, assessment of healing, and discussion of further treatment or monitoring, such as radiation therapy, chemotherapy, or even possible clinical trials.
Cognition After Brain Surgery
It’s common after brain surgery to have at least a subtle change to the way people think, called cognition, particularly if surgery occurred near speech or language areas.
“We expect that subtle change to feel worse on the second or third day after surgery,” said Amy Maguire, MS, CCC-SLP, of the MGH SLP Brain Tumor Team. “In general, it should be improving over the next month.”
If patients are experiencing cognition changes as a symptom leading up to surgery, those difficulties can sometimes linger in the initial aftermath of surgery.
“It can fluctuate a lot with attention because attention is maybe the major thing that changes after surgery,” Amy said. “I like to tell people it’s almost like the filter that you’ve been using before to focus on one thing and ignore others is a little bit less airtight. The brain is more prone to distraction and fatigue. Generally speaking, that’s what we want people to flag for themselves the most.”
Instead of having a conversation with three people at the same time as someone might do before surgery, patients are encouraged to try to focus on a conversation with one person at a time and pace themselves with the length of the conversation. For example, when a patient returns from the hospital, a large gathering at home might tap them out within 10 minutes.
Speech and Language After Brain Surgery
“A majority of our patients have some residual language difficulties, especially with word finding,” said Sarah Steele, MS, CCC-SLP, of the MGH SLP Brain Tumor Team.
After Julio P.’s craniotomy, he worked with an SLP and a neuropsychologist to address some of his communication challenges.
“There was a little deficit with word finding,” Julio’s wife, Liz, said. “She was helping him with strategies to cope with that. The neuropsychologist at the University of California San Francisco helped give tricks and tips to get around little deficits while he built that back up.”
It is important for patients to advocate for themselves when they can and for friends, family, and other acquaintances to remember they are still navigating speech and language challenges long after the surgery scar has healed.
“Communicating with people at home is where we find that patients express the most frustration,” Sarah said. “I think that’s where we find people express the most frustration because it’s like an invisible cognitive or language change to their family members or friends. Many patients mention when their hair grows back over their surgery scar, and it’s not as noticeable anymore, that people aren’t as patient with them because it’s not as apparent that they might be having some of the challenges they are.”
Next Up: Tips from Patients and Care Partners
In part two of our brain surgery series, hear from patients and care partners as they share tips based on their personal surgery experiences.
The content on this website is for informational and educational purposes only. It does not constitute medical advice. Always consult a professional for your particular needs and circumstances before making medical, professional, legal, or financial decisions.